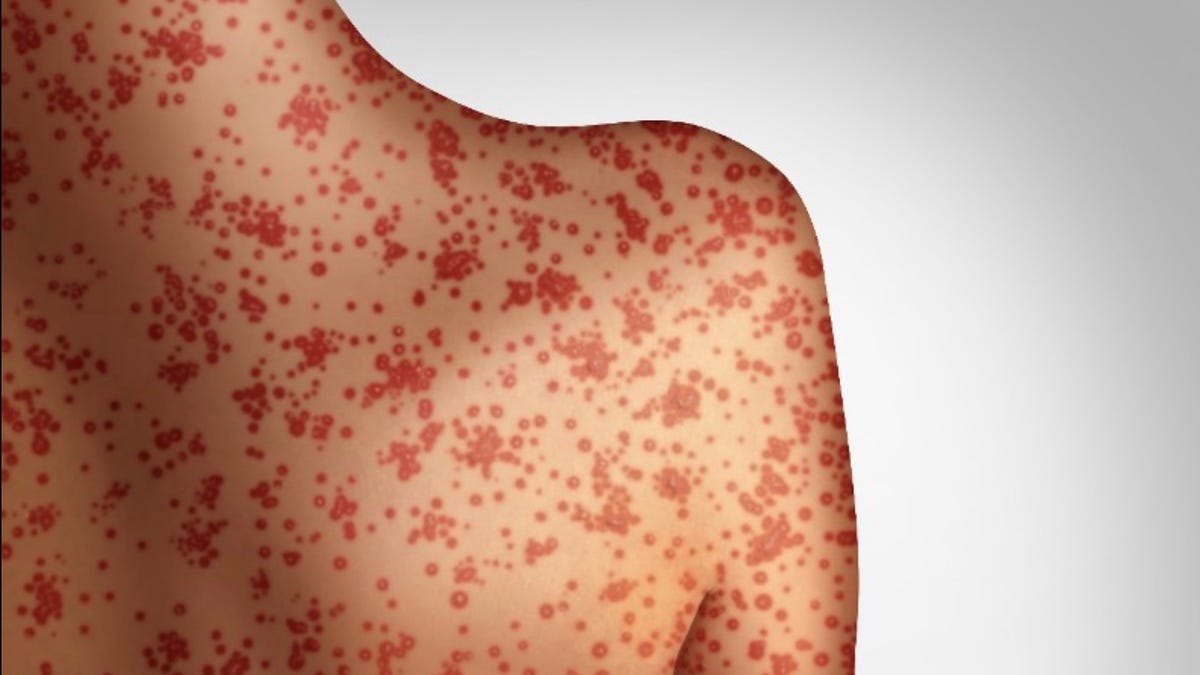
Rising Measles Cases and the Decline of Vaccination Rates in the US: A Concern for Public Health
In recent years, the anti-vax movement has gained traction in the United States, leading to a surge in measles outbreaks. These outbreaks have occurred in various states, prompting officials to…
Trump’s High Stakes in Truth Social: Will Investment Dilemma Derail Election Campaign?
As the US presidential election approaches, Donald Trump is turning to social network Truth Social in an attempt to raise funds for his campaign. However, the investment in this venture…
Tesla Cybertrucks Recalled Due to Stuck Accelerator Pedal: 4,000 Vehicles Affected and Repair Required
The US National Highway Traffic Safety Administration (NHTSA) has ordered Tesla to recall nearly 4,000 of its Cybertrucks due to an accelerator pedal that can become stuck when pressed down.…
Santa Rosa’s Biggest Bounce House in the World
The “World’s Largest Bounce House” and six other massive inflatable attractions will be making a stop in Santa Rosa this weekend. The Big Bounce America tour will take place at…
Baker Technology Provides Responses to Shareholder Inquiries Ahead of AGM Meeting
Baker Technology Limited (SG:BTP) has recently provided an update to its shareholders. The company would like to thank its shareholders for their participation and engagement, particularly in submitting questions ahead…
Discovering the Latest Innovations in the WorldTour with POC Sports: A Podcast Exploration
Alison has captivated audiences with her dance moves on social media and on various platforms. Her passion for movement, whether it’s dancing, horseback riding, or exploring the outdoors, is truly…
Purdue University Researchers Earn Prestigious AAAS Fellowship: Advancing Science Through Dedication and Innovation
Purdue University has received recognition from the American Association for the Advancement of Science, as several faculty members have been selected as fellows. This prestigious award highlights the contributions made…
Boosting Girls’ Confidence: RUSH Program Launches with Flag Football at UNLV
Nearly 100 middle school girls were introduced to flag football through the RUSH program at the UNLV Peter Johann Memorial Soccer Field in Las Vegas. Funded by the Las Vegas…
Economic Optimism vs. Reality: Unraveling the Disparity in Iowa
Despite positive indicators such as low unemployment rates, abundant job opportunities, and economic growth in Iowa, a significant portion of the population holds a pessimistic outlook on the state of…
Seritage Growth Properties Announces Plan to Sell Off Assets and Return Proceeds to Investors: The Motley Fool’s Matt Frankel Weighs in
In light of the challenges faced during the COVID-19 pandemic, Seritage Growth Properties has decided to sell off its assets and return the proceeds to investors. Despite a low stock…